

In recent years, the rapid adoption of computer-based techniques for surgical planning and visualization and image-guided surgery has made possible a number of impressive advances in functional neurosurgery.
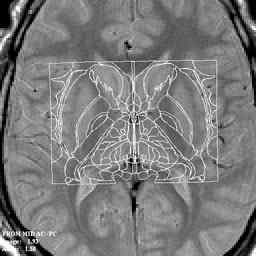 Magnetic resonance imaging (MRI) allows the acquisition of highly detailed structural information
about the soft tissues of the brain. Minute pathological alterations can be visualized, even before they can be
detected by other means. Stereotactical atlases based on this information are now used to achieve an exquisite
precision of location of the electrodes and probes and for planning the operation.
Magnetic resonance imaging (MRI) allows the acquisition of highly detailed structural information
about the soft tissues of the brain. Minute pathological alterations can be visualized, even before they can be
detected by other means. Stereotactical atlases based on this information are now used to achieve an exquisite
precision of location of the electrodes and probes and for planning the operation.
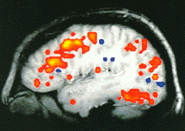 Functional imaging is also now also possible utilizing special metabolic markers and MRI,
and computerized techniques for mathematical processing and visualization of the images. In this way, non-invasive
evaluation of brain function in epilepsy, Parkinson's disease and other brain conditions can be performed with
extraordinary precision and sensitivity.
Functional imaging is also now also possible utilizing special metabolic markers and MRI,
and computerized techniques for mathematical processing and visualization of the images. In this way, non-invasive
evaluation of brain function in epilepsy, Parkinson's disease and other brain conditions can be performed with
extraordinary precision and sensitivity.
In order to facilitate image-guided surgery, there is a number of companies which already offer small intraoperative MRI systems.

 The stereotactic
technique has been improved in precision and sophistication, and now includes laser endoscopy, computer-driven
guidance systems, techniques of visualization based on virtual reality and even surgical robots which have a higher
precision than the human hand. A new technique called frameless stereotaxis, dispenses with the external metallic
frame used to locate the brain points by means of coordinates, and, instead, uses computerized calculations based
on visible landmarks in the MRI images.
The stereotactic
technique has been improved in precision and sophistication, and now includes laser endoscopy, computer-driven
guidance systems, techniques of visualization based on virtual reality and even surgical robots which have a higher
precision than the human hand. A new technique called frameless stereotaxis, dispenses with the external metallic
frame used to locate the brain points by means of coordinates, and, instead, uses computerized calculations based
on visible landmarks in the MRI images.
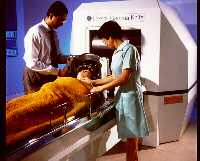
 Stereotactic surgery without
opening the skull and without blood (even the patient's head doesn't need to be shaved) is possible with a revolutionary
technique called radiosurgery. The destruction of nervous or vascular tissue inside the brain is achieved by projecting
thin and powerful beams of ionizing radiation, coming from several angles around the patient's head. They are produced
by linear accelerators, machines used in high energy particle physics, or by sources of radioactive cobalt (the
"gamma knife", developed in the 60s by the Swedish neurosurgeon Lars Leksell). In this way, radiation energy concentrates into a single, small point inside the brain,
while the surrounding, healthy tissues are spared damage.
Stereotactic surgery without
opening the skull and without blood (even the patient's head doesn't need to be shaved) is possible with a revolutionary
technique called radiosurgery. The destruction of nervous or vascular tissue inside the brain is achieved by projecting
thin and powerful beams of ionizing radiation, coming from several angles around the patient's head. They are produced
by linear accelerators, machines used in high energy particle physics, or by sources of radioactive cobalt (the
"gamma knife", developed in the 60s by the Swedish neurosurgeon Lars Leksell). In this way, radiation energy concentrates into a single, small point inside the brain,
while the surrounding, healthy tissues are spared damage.
Despite all this technical progress, however, psychosurgery is practiced less and less. The problem is no longer a technical one; or a lack of knowledge of what to do. The problem is of ethical and political nature. Psychosurgery will never be performed "en masse" as the old lobotomy, without evaluation of precise indication. There are a number of guidelines and safeguards in place, which will assure, at least in democratic countries, that the rights of the citizens will be respected in regard to the possibility of undergoing brain surgery for the treatment of mental diseases.
| From: The History of Psychosurgery Author: Renato M.E. Sabbatini, PhD Source: Brain & Mind Magazine, June 1997 |