
|
|
[ Diagnosis |Causes | Treatment | To Know More | Credits ]
Terrifying dreams are part of human nature: there are very few persons who have never had a nightmare sometime in life. As the picture above shows, the ancient Greeks even thought that during nightmare one is dominated by an "incubus" (a small demon) who sits on the dreamer's chest, leading to a sense of suffocation, breath difficulties, a racing and heavy heart.
However, there is a rare type of frightening phenomenon during sleep which is not quite like a nightmare. It is called "night terrors" or "Pavor Nocturnus" and it is a severe sleep disturbance, consisting of attacks of acute terror arising in deep sleep without dreaming. It is accompanied by violent body movements, extreme agitation, gasping, moaning, screaming, sweating, confusion, and in some cases, flight from the bed or the room, destructive behavior and aggression directed toward objects or against themselves or other persons. Wounds, fractures and lesions may occur in consequence.
Sleep terrors occur during a phase of deep non-REM (Rapid Eye Movement) sleep usually within an hour after the subject goes to bed (stage 4). An episode may last anywhere from five to twenty minutes while the subject is still asleep. The eyes may be open. The patient is unable to recall anything afterwards.
Sleep terrors may coincide with sleepwalking (in fact, one third of children with night terrors also have somnambulism), in which case walking or running occur in conjunction with shouting, jumping and thrashing about. Milder episodes, called "confusional arousals" are more common in children, and may involve only moaning, muttering, and motor agitation of the head, body and legs. After the episode, the patient cannot be consoled, and is unaware of nearby people or surroundings.
During a terror atack, there is an overactivity of the sympathetic autonomous nervous system, including large pupils, sweating, increase in the heart and respiration rates, and increased blood pressure. The heart rate (tachycardia) may increase to 160 to 170 beats per minute, which is higher than those occurring during the most severe stress episodes.
The following are still images of
a man filmed during a night terrors atack in a research laboratory in the
USA
 |
 |
 |
 |
 |
 |
According to DSM-IV international classification of psychological disorders, the following are the criteria used to diagnose the sleep terror disorder:
Night terrors are a type of parasomnia (unusual occurrences during sleep, such as inappropriate movements and behaviors). The most common parasomnias are paroxysmal in nature ("attacks"), and these include night terrors, nightmares, sleepwalking (somnambulism) and bedwetting (enuresis). The causes of night terror are still unknown, but it is believed to be physiological, not psychological. Intense anxiety, stress and conflicts, either conscious or subconscious, are a facilitating factor. In children, precipitating traumatic events, febrile illness and emotional disorder may play a role.
Nightmares and night terrors are not the same thing, because nightmares are disturbances of dreaming and occur during the REM (rapid eye movement) stage of sleep; while night terrors do not have this association, and occur in the stages 3 and 4 of deep sleep. Nightmares are easily recalled and do not lead to mental confusion and disorientation, sleep-walking and other phenomena which are typical of night terrors. Besides night terror, two other disorders, sleepwalking and bed-wetting, usually occur during stage 4 of sleep, and not during dreaming. The resting EEG of night terror patients is usually normal.
However, night terrors may be influenced by anything that prolongs or intensifies REM sleep, such as abrupt shifts in the sleep-wake rhythm, and also by the deprivation of the deeper sleep stages (3 and 4). Sometimes they arise in patients who are taking antidepressant medications and stop them (these medications, such as tricyclic antidepressants and monoamine oxidade inhibitors, are known to suppress REM sleep).
Some biological theories of night terror point out to an immaturity of the nervous system as a possible cause, but this has not been proven. However, it is true that it is more frequent in children between the ages of three and five. From 1 to 4% of children show at least recurring episodes and male children are more affected than female. In children, it is usually a self-limiting disorder, which disappear spontaneously after a few episodes.
Adults have it too, though, and some of them may experience it weekly, and sometimes several nights in a row. In adults, the disorder may take years to disappear and treatment is more difficult.
There is no evidence of genetic factors, but sometimes susceptibility to night terrors run in families.
Minimizing stress and predisposing factors, such as irregularities of time of going to bed and awakening, eating spicy or fatty foods before going to bed, etc., should be tried first. In the case that the patient is taking any predisposing drug, it should be suspended gradually. Long term psychotherapy is often necessary. Hypnosis and biofeedback techniques may help too. Certain psychoactive drugs such as tricyclic antidepressants (imimaprine) and benzodiazepines (diazepam) may be used for the short term control of night terrors, but their result is uncertain and should be avoided when possible.
 Treatment
should aim also at protecting the patient from possible damage to himself
and others. Interpersonal aggression may be avoided by sleeping alone.
Electronic devices have been used to awake the patient with a loud audible
alarm when body movement indicative of an episode of night terror occurs.
An electronic engineer, after one such episodes, when he destroyed the
furniture and appliances in his room and broke one arm, invented an "electric
eye" for this: an invisible infrared beam placed 30 cm above the bed,
which is interrupted when the patient sits up, and starts an alarm. Closing
the door and windows from the outside also helps to prevent patients to
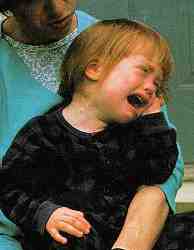
leave the room during night terrors episodes. Children may be held soothingly
but firmly in the caretaker's arms and lap and spoken softly to, until
the terrors decrease.
Treatment
should aim also at protecting the patient from possible damage to himself
and others. Interpersonal aggression may be avoided by sleeping alone.
Electronic devices have been used to awake the patient with a loud audible
alarm when body movement indicative of an episode of night terror occurs.
An electronic engineer, after one such episodes, when he destroyed the
furniture and appliances in his room and broke one arm, invented an "electric
eye" for this: an invisible infrared beam placed 30 cm above the bed,
which is interrupted when the patient sits up, and starts an alarm. Closing
the door and windows from the outside also helps to prevent patients to
leave the room during night terrors episodes. Children may be held soothingly
but firmly in the caretaker's arms and lap and spoken softly to, until
the terrors decrease.
 Silvia Helena Cardoso, PhD. Psychobiologist, master and doctor in Sciences. Director and editor-in-chief of Brain & Mind. State University of Campinas, Campinas, Brazil. |
 Renato M.E. Sabbatini, PhD. director of the Center for Biomedical Informatics and Chairman of Medical Informatics of the Medical School of the State University of Campinas, Campinas, Brazil. |